A lower risk of moderate exacerbations was observed with the FDC compared to formoterol but not with the FDC compared with aclidinium. There was no difference between the FDC and monotherapy or placebo for hospital admissions, mortality, and non-fatal adverse events. Quality of life (SGRQ) was better with the combination compared to formoterol or placebo. In a systematic review of seven trials ( Ni 2018), the aclidinium/formoterol fixed dose combination (FDC) was found to improve dyspnoea and lung function compared to the monocomponents or placebo. Aclidinium/formoterol reduced the rate of moderate to severe exacerbations by 29%, when compared to placebo, but not when compared to aclidinium or formoterol alone ( Bateman 2015). There were some improvements in dyspnoea and health-related quality of life (HRQoL), measured by St George’s Respiratory Questionnaire (SGRQ). glycopyrronium/indacaterol (Breezhaler)Īclidinium/formoterol: Twice daily aclidinium/formoterol had greater bronchodilation over placebo (mean FEV 1 up to 143 ml greater), and to a lesser extent, versus formoterol (mean FEV 1 53 ml greater) or aclidinium (small differences at various timepoints) ( Bateman 2015, D’Urzo 2014, Singh 2014b).O1.2.3 Long-acting bronchodilator combinations (LAMA/LABA)Ī number of LAMA/LABA fixed dose combinations in a single inhaler are available in Australia, which are delivered via a range of devices: All Papers Considered for Citation in COPD-X.Appendix 6: Table of Systematic Reviews Evaluating the Effect of Self-Management in COPD.Appendix 5 – Table of Minimum Clinically Important Differences (MCID).Appendix 4 – Strategies that may assist in reminding people to reduce sedentary time.Appendix 2 – Explanation of inhaler devices.Appendix 1 – Use and doses of long-term inhaled bronchodilator and corticosteroids determined in response trials.Uptake and impact of guidelines for exacerbations X3.5 Develop post-discharge plan and follow-up.X3.2.1 Humidified nasal high flow therapy (hNHF).Refer appropriately to prevent further deterioration (‘P’) X2.2.4 Combined systemic corticosteroids and antibiotics for treatment of exacerbation.X2.2.3 Antibiotics for treatment of exacerbations.X2.2.2 Systemic corticosteroids for treatment of exacerbations.X2.2.1 Inhaled bronchodilators for treatment of exacerbations.X2.1 Confirm exacerbation and categorise severity.Assessment and management of anxiety and depression D1.7 Clinical psychologist/psychiatrist.D1.3 GP practice nurse/ nurse practitioner/ respiratory educator/ respiratory nurse.P11 Long-term home non-invasive ventilation.Humidification therapy and nasal high flow (NHF) therapy P2.3 Haemophilus influenzae immunisation.P1.2.5 Electronic cigarettes (e-cigarettes).P1.2.2 Nicotine Receptor Partial Agonists.O10.3 Palliative oxygen therapy for dyspnoea.O9.2 Lung volume reduction surgery and bronchoscopic interventions.O8.1 Treatment of hypoxaemia and pulmonary hypertension.O7.13 Testosterone deficiencies and supplementation.O7.11 Combined pulmonary fibrosis and emphysema.O7.8 Gastro-oesophageal reflux disease (GORD).O7.2.5 Coronary revascularisation procedures.O7.1 Increased risks from comorbidities in the presence of COPD.O6.8 Chest physiotherapy (Airway clearance techniques).O6.5 Physical activity and sedentary behaviour.O6.4 Neuromuscular Electrical Stimulation.O4.2.1 Eosinophil count and inhaled corticosteroids.O4.2 Inhaled corticosteroids and long-acting beta2-agonists and long-acting antimuscarinics in combination.O4.1 Inhaled corticosteroids and long-acting beta2-agonists in combination (ICS/LABA).O3.3 Inhaled corticosteroids versus long-acting beta2-agonists.O2.2 Phosphodiesterase type-4 inhibitors.O1.3 Assessment of response and continuation of bronchodilator therapy.O1.2.3 Long-acting bronchodilator combinations (LAMA/LABA).O1.2.2 Long-acting beta2-agonists (LABA).O1.2.1 Long-acting muscarinic antagonists (LAMA).O1.1.3 Short-acting bronchodilator combinations.O1.1.2 Short-acting muscarinic antagonist (SAMA).O1.1.1 Short-acting beta2-agonists (SABA). 
C5.11 Electrocardiography and echocardiography.C5.5 High resolution computed tomography.Assessing acute response to bronchodilators Key Recommendations of the COPD-X Guidelines.COPD Guidelines Committee – Past and Present.Summary of the Changes from the previous three versions of COPD-X.Summary of the major changes – Version 2.71, July 2023. 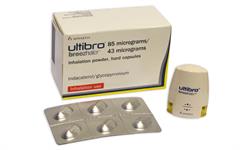
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
